Paediatric assessment
Continually monitor paediatric patients
Since XLH is a chronic, progressive skeletal disorder,1-4 continual assessment is needed from childhood through adulthood to monitor the effects.5 Children should also be asked to identify areas of pain that may not show up during office visits.
Monitoring and dose adjustment at 3-month intervals are recommended to avoid hypercalcaemia, hypercalciuria, nephrocalcinosis, and hyperparathyroidism5
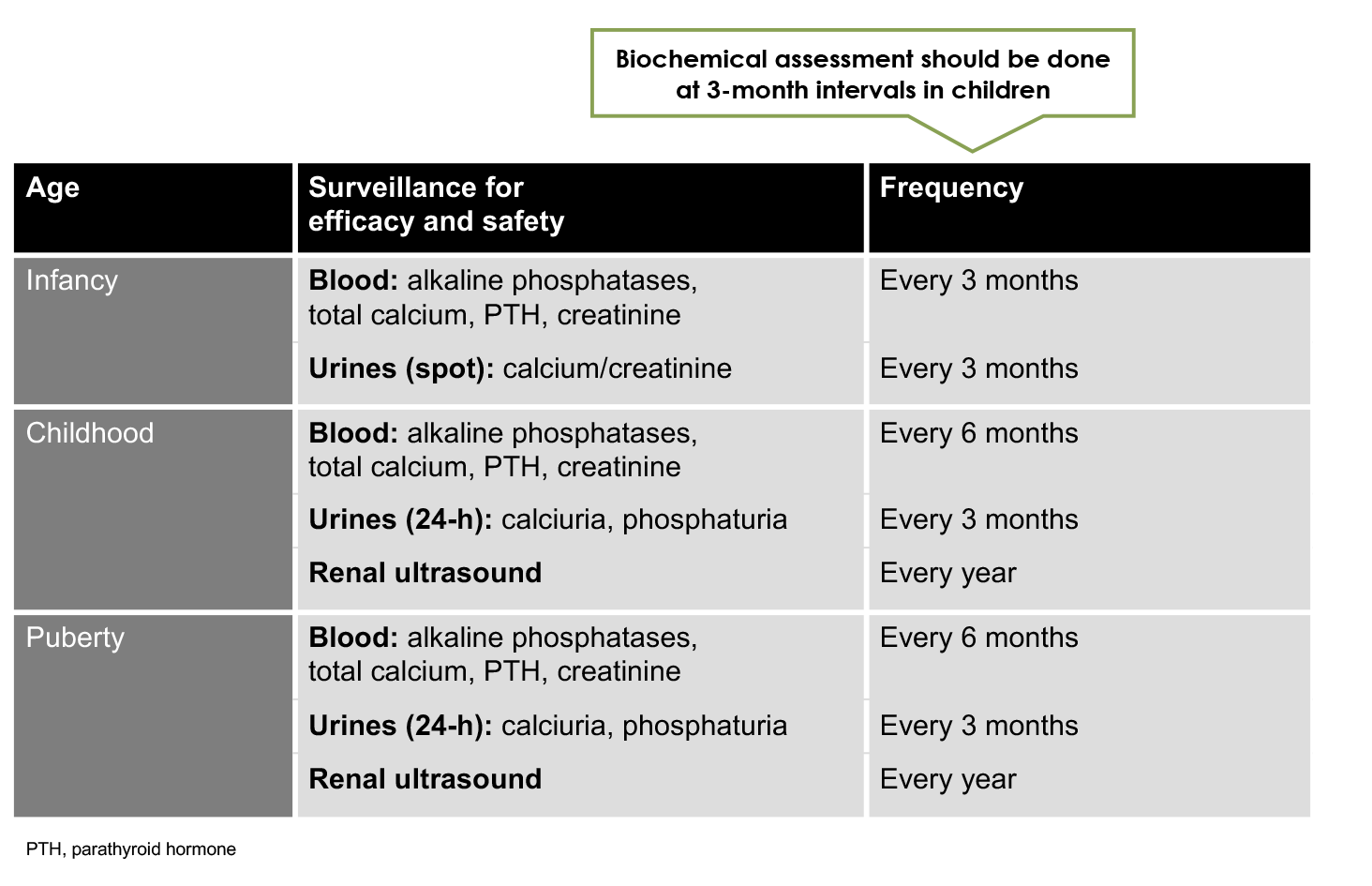
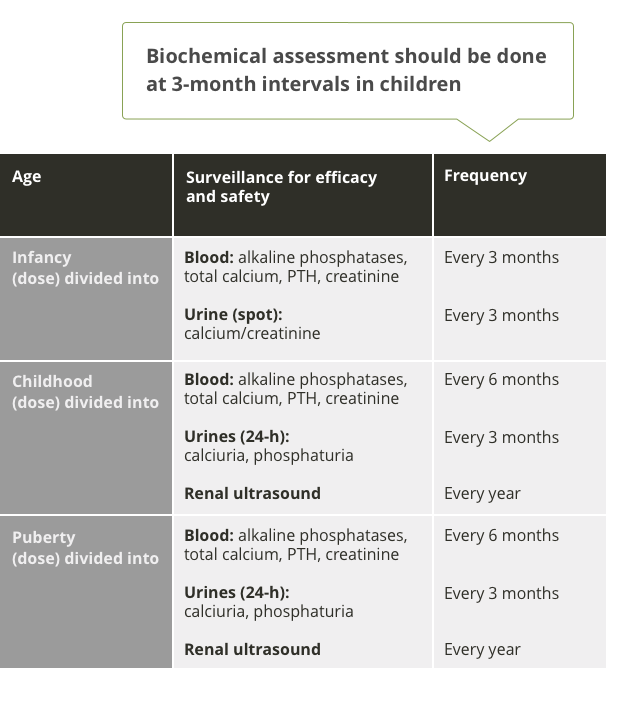
Skeletal assessment for paediatric patients with XLH
XLH is a chronic, progressive disease, with lower limb deformity, loss of growth potential, and body disproportion increasing with age. Children should be routinely assessed for safety and response to medical treatment.6,7
Anthropometric measurements
To ensure standardised and comparable results, it is recommended that all anthropometric measurements are performed by the same health care provider.9
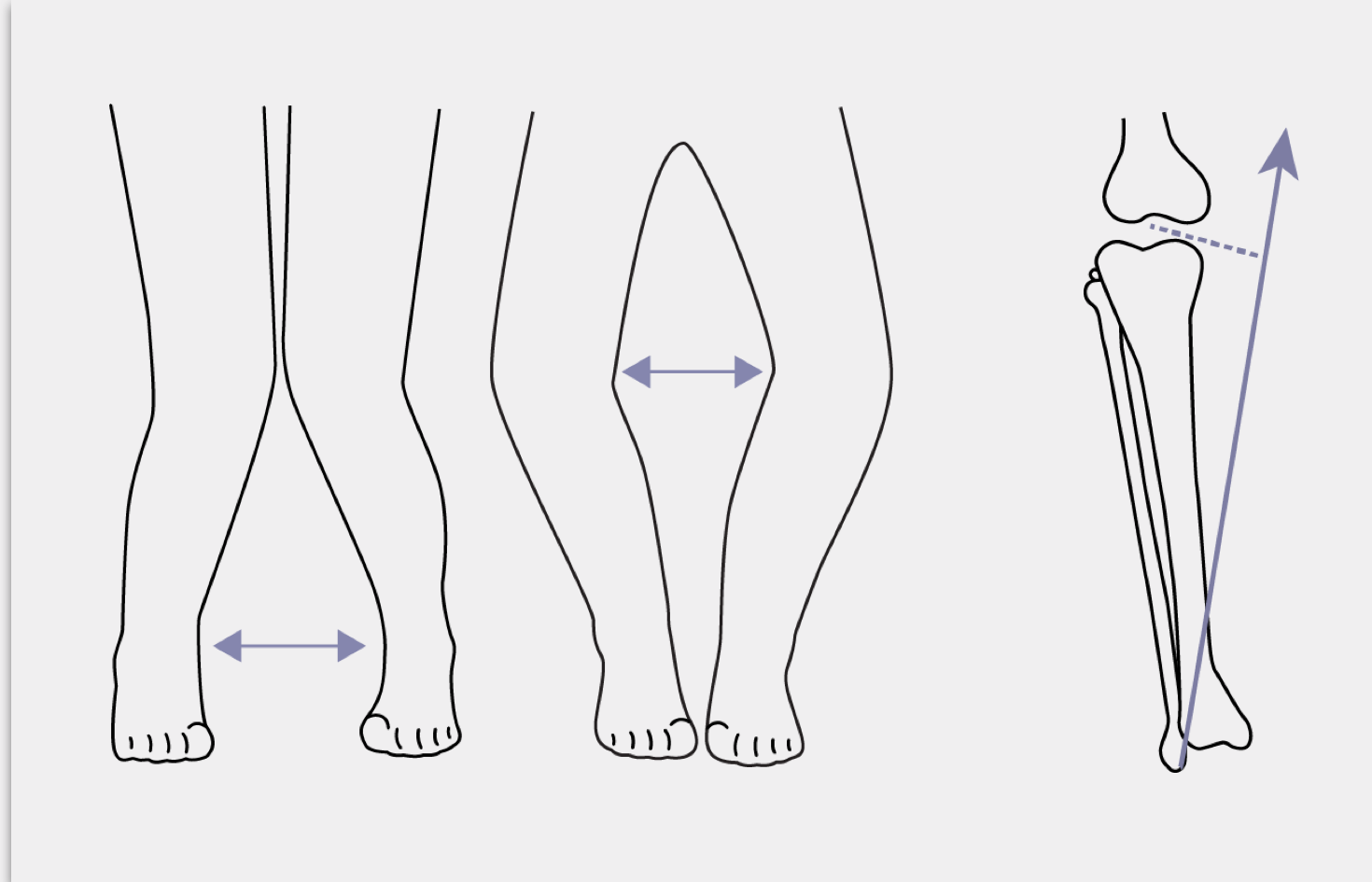
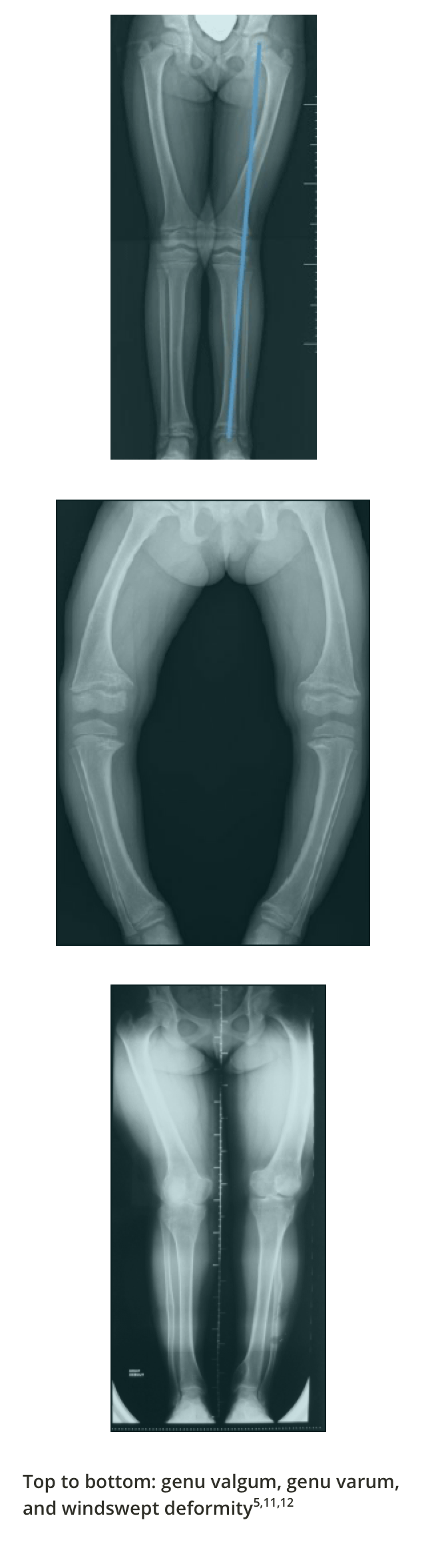
Tibiofemoral angle
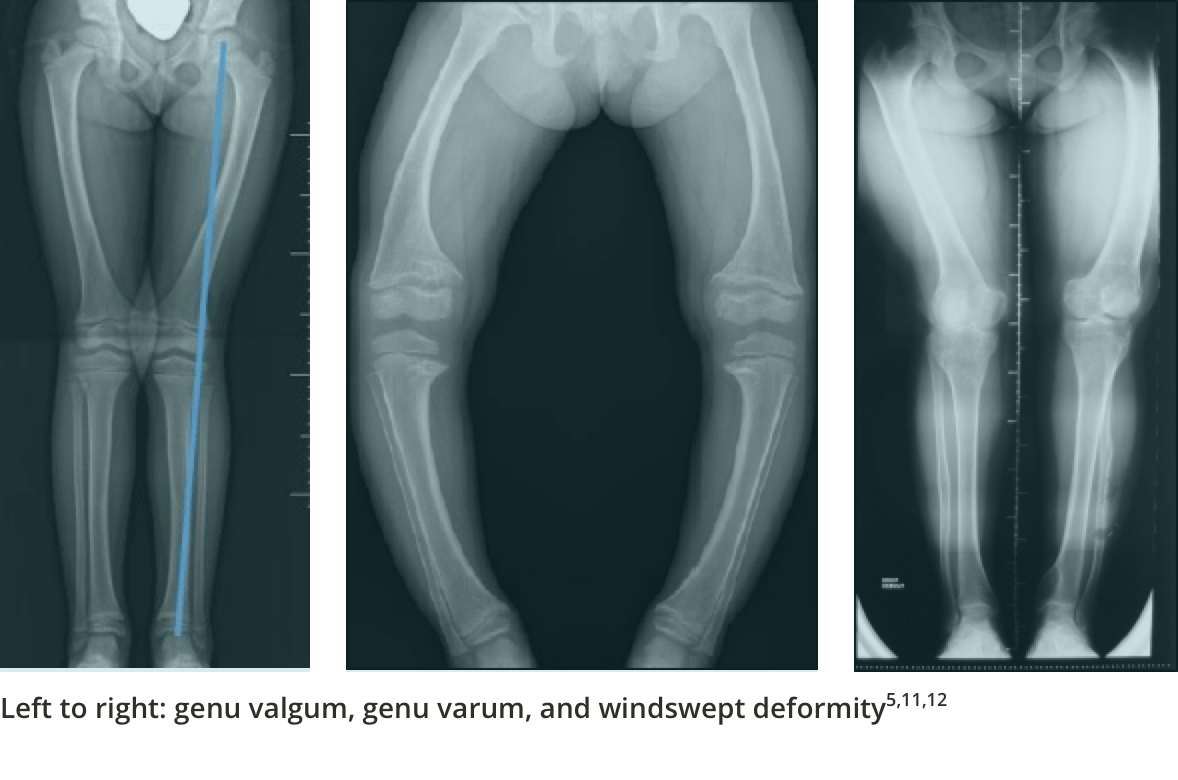
The tibiofemoral angle can be clinically assessed by the intercondylar and intermalleolar distances. A variation becomes a deformity when the amount of deviation from normal for that particular age is >2 SD. Response to conventional therapy is defined as a 1-cm decrease in genu valgum or genu varum every 6 months.5,10
Age-related growth and proportion evaluation is comprised of different assessments: standing and sitting height, and arm and leg length.9
Leg length should be measured as standing height versus
sitting height.9
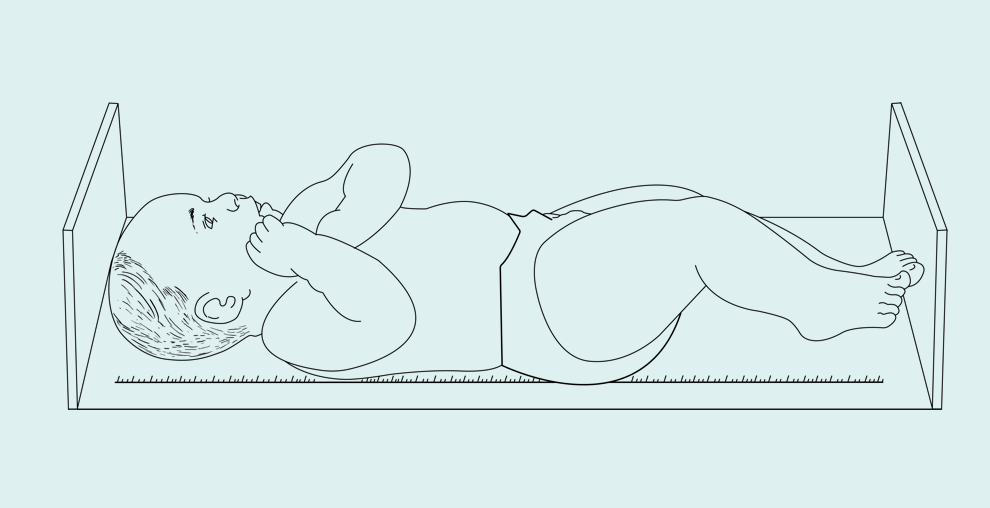
Recumbent Length
Two people are required to measure recumbent length. The patient’s head is positioned on a fixed headboard, while the feet are positioned and the footboard adjusted for measurement.
The child is placed supine on the infant board with buttocks and shoulder blades in contact with the board. The child should be measured with minimal clothing. The Frankfort horizontal plane13 should be parallel to the head and foot boards. The patient’s head should be up and their eyes facing forward. Gentle pressure should be applied to the legs to prevent the knees from flexing, while the footboard is adjusted until it rests firmly against the child’s heels.
Growth
Children with XLH generally show disproportionate growth, so regular measurement and assessment are important.9
Height-for-age Z-score: Growth Z-scores reflect the number of standard deviations from age- and sex-matched normal mean values.14
- Z-scores are based on standard growth references collected from normal children
- The WHO recommends cutoff Z-score values of ±2 to define abnormal growth
- Short stature is defined as height-for-age Z-scores <–2 for individuals of the same sex


Rickets often causes lower-extremity deformity and loss of growth potential.6
Because of open epiphyses, patients present a significant risk of recurrent bowing at the level of osteotomy or secondary to adjacent epiphysiodesis.5
Quality of life and physical function for paediatric patients with XLH
Several different tools are available to assess quality of life and physical function
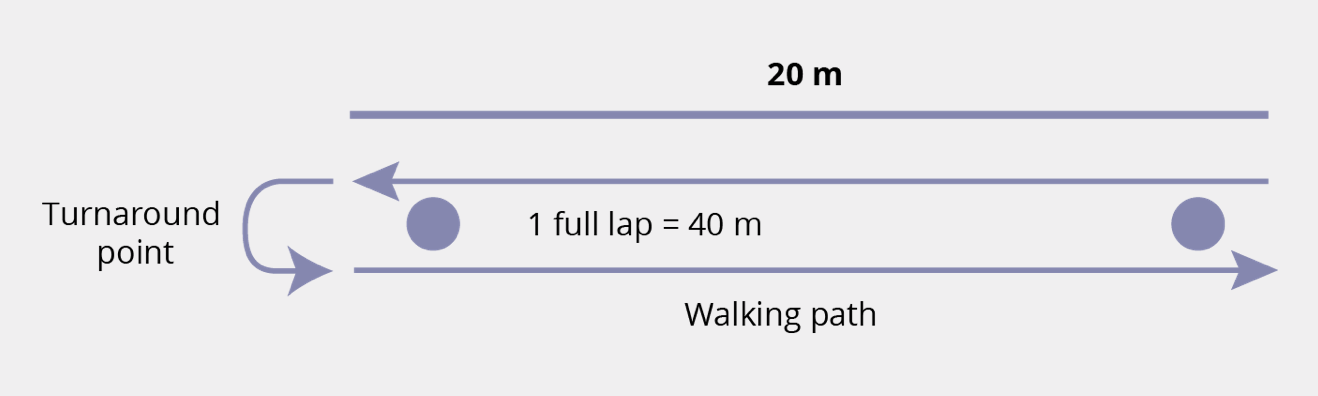
6-minute walk test (6MWT)15
The 6MWT is a practical, simple test that measures how far a patient can walk in 6 minutes on a flat, hard surface.
POSNA PODCI16
A parent-completed questionnaire to assess overall health, pain and ability to participate in normal daily activities, as well as in more vigorous activities associated with young people.
PROMIS (Patient-Reported Outcomes Measurement Information System)17
PROMIS was developed by the NIH and uses domain-specific measures to assess physical, mental, and social health.
SF-1018
The SF-10 for Children™ is a short-form survey that contains items adapted from the CHQ (Child Health Questionnaire) and scored to produce physical (PHS) and psychosocial health (PSS) summary scores.
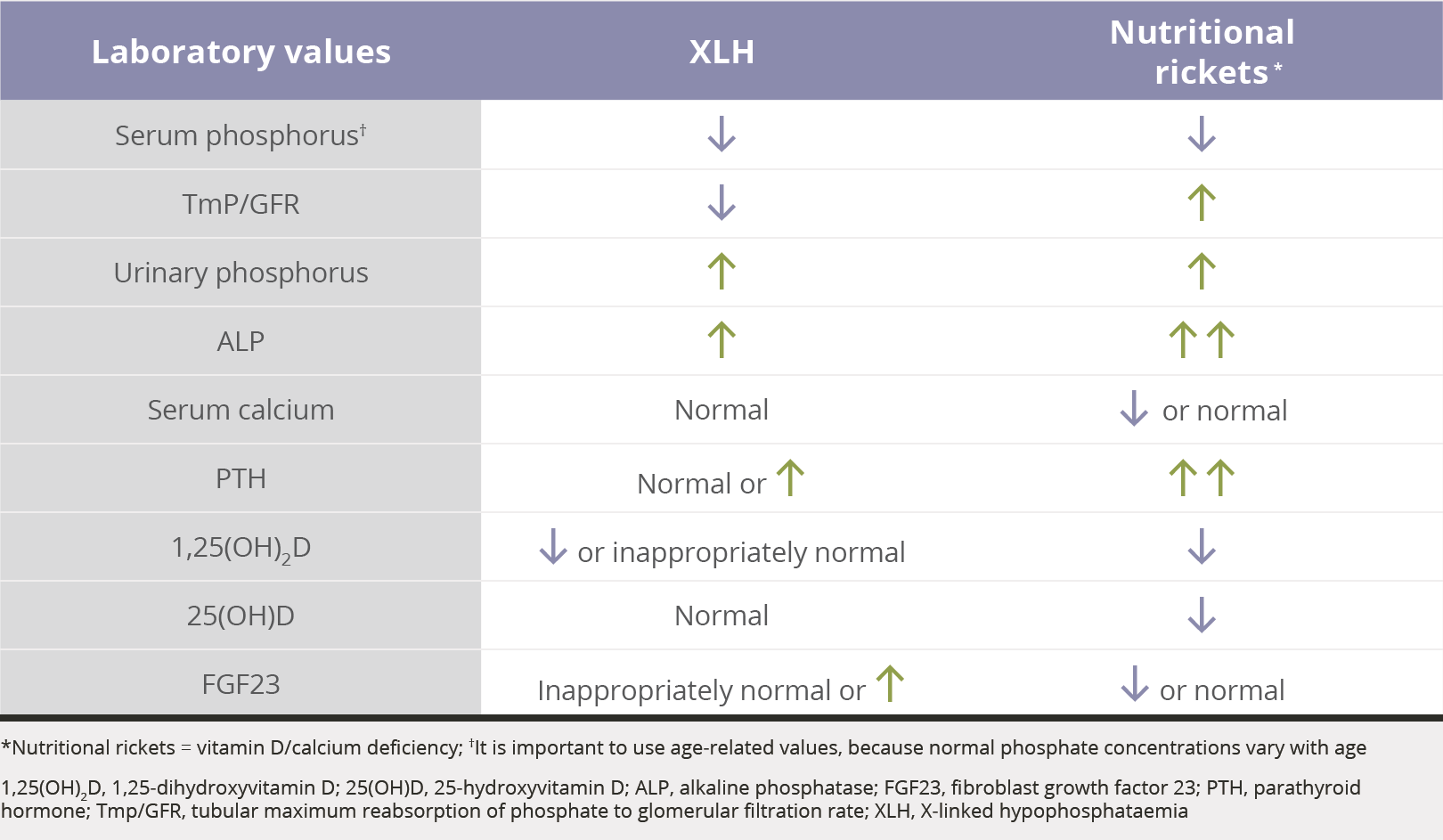
Measuring
The TmP/GFR is the ratio of renal tubular maximum reabsorption of phosphate (TmP) to glomerular filtration rate (TmP/GFR).6,20-25



1. Beck-Nielsen SS, Brock-Jacobsen B, Gram J, Brixen K, Jensen TK. Incidence and prevalence of nutritional and hereditary rickets in southern Denmark. Eur J Endocrinol. 2009;160(3):491-497. 2. Martin A, Quarles LD. Evidence for FGF23 involvement in a bone-kidney axis regulating bone mineralization and systemic phosphate and vitamin D homeostasis. Adv Exp Med Biol. 2012;728:65-83. 3. Che H, Roux C, Etcheto A, et al. Impaired quality of life in adults with X-linked hypophosphatemia and skeletal symptoms. Eur J Endocrinol. 2016;174(3):325-333. 4. Carpenter TO, Imel EA, Holm IA, Jan de Beur SM, Insogna KL. A clinician's guide to X-linked hypophosphatemia. J Bone Miner Res. 2011;26(7):1381-1388. 5. Linglart A, Biosse-Duplan M, Briot K, et al. Therapeutic management of hypophosphatemic rickets from infancy to adulthood. Endocr Connect. 2014;3(1):R13-R30. 6. Ruppe MD. X-linked hypophosphatemia. In: Pagon RA, Adam MP, Ardinger HH, et al, eds. Gene Reviews. https://www.ncbi.nlm.nih.gov/books/NBK83985/. Accessed October 20, 2017. 7. Pettifor JM. What's new in hypophosphataemic rickets? Eur J Pediatr. 2008;167(5):493-499. 8. Penido MG, Alon US. Phosphate homeostasis and its role in bone health. Pediatr Nephrol. 2012;27(11):2039-2048. 9. Zivičnjak M, Schnabel D, Billing H, et al. Age-related stature and linear body segments in children with X-linked hypophosphatemic rickets. Pediatr Nephrol. 2011;26(2):223-231. 10. Sass P, Hassan G. Lower extremity abnormalities in children. Am Fam Physician. 2003;68(3):461-468. 11. Stevens NM, Hennrikus WL. 3 cases of genu valgum in medically treated X-linked hypophosphatemic rickets. Austin J Orthop Rheumatol. 2015;2(3):1-3. 12. Gizard A, Rothenbuhler A, Pejin Z, et al. Outcomes of orthopedic surgery in a cohort of 49 patients with X-linked hypophosphatemic rickets (XLHR). Endocr Connect. 2017;6(8):566-573. 13. Frankfort horizontal plane. Merriam Webster Medical Dictionary Online Web site. https://www.merriam-webster.com/medical/Frankfort%20horizontal%20plane. Accessed October 17, 2017. 14. de Onis M, Blössner M. WHO Global Database on Child Growth and Malnutrition. Geneva, Switzerland: World Health Organization; 1997. 15. Geiger R, Strasak A, Treml B, et al. Six-minute walk test in children and adolescents. J Paediatr. 2007;150(4):395-399. 16. Daltroy LH, Liang MH, Fossel MH, et al. The POSNA Paediatric Musculoskeletal Functional Health Questionnaire: report on reliability, validity, and sensitivity to change. J Paediatr Orthop. 1998;18(5):561-571. 17. Broderick JE. Advances in patient-reported outcomes: the NIH PROMIS measures. eGEMS. 2013;1(1):1015. 18. Saris-Baglama RN, DeRosa MA, Raczek AE, et al. Preliminary validation of the SF-10v2 for Children among those with and without disabilities. Poster presented at the American Public Health Association 134th Annual Meeting and Exposition; November 4–8, 2006. Boston, MA. 19. Hicks C, von Baeyer C, Spafford P, et al. The FACES Pain Scale - revised: toward a common metric in paediatric pain measurement. Pain. 2001;93(2):173-183. 20. Payne RB. Renal tubular reabsorption of phosphate (TmP/GFR): indications and interpretation. Ann Clin Biochem. 1998;35(pt. 2):201-206. 21. Santos F, Fuente R, Mejia N, Mantecon L, Gil-Peña H, Ordoñez FA. Hypophosphatemia and growth. Pediatr Nephrol. 2013;28(4):595-603. 22. Goldsweig BK, Carpenter TO. Hypophosphatemic rickets: lessons from disrupted FGF23 control of phosphorus homeostasis. Curr Osteoporos Rep. 2015;13(2):88-97. 23. Imel EA, Carpenter TO. A practical clinical approach to paediatric phosphate disorders. Endocr Dev. 2015;28:134-161. 24. Özkan B. Nutritional rickets. J Clin Res Pediatr Endocrinol. 2010;2(4):137-143. 25. Nield LS, Mahajan P, Joshi A, Kamat D. Rickets: not a disease of the past. Am Fam Physician. 2006;74(4):619-626. 26. Haffner D, Emma F, Eastwood DM, et al. Clinical practice recommendations for the diagnosis and management of X-linked hypophosphataemia. Nat Rev Nephrol. 2019;15(7):435-455.